How the One Big Beautiful Bill Could Hurt Evansville Families—and the Hospitals That Treat Them
New Medicaid work requirements and funding caps under the One Big Beautiful Bill Act may push more Evansville residents off coverage while forcing local hospitals and clinics to do more with less.

New Medicaid work requirements and funding caps under the One Big Beautiful Bill Act may push more Evansville residents off coverage while forcing local hospitals and clinics to do more with less.
By Rasheedah Ajibade
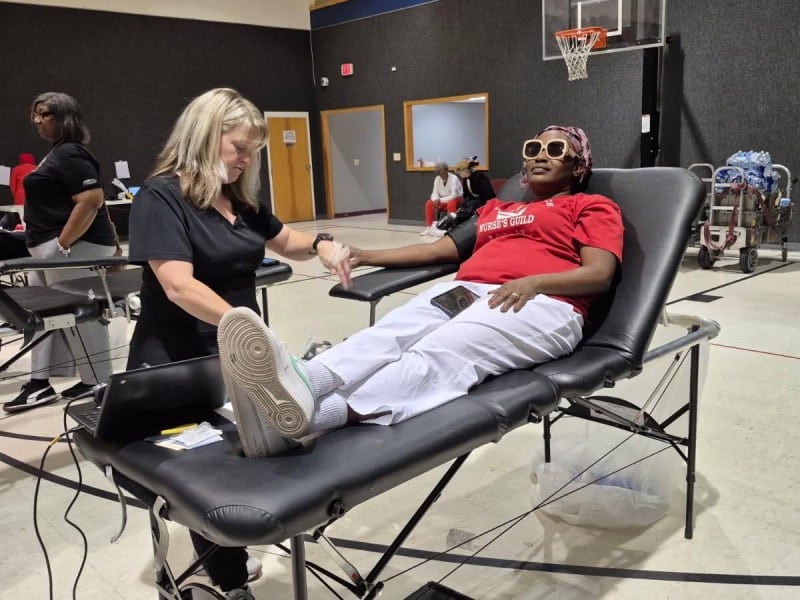
Last Saturday at the CK Newsome Center in Evansville, a coalition of local groups hosted “Medicaid Matters: First Aid for Your Insurance,” a forum to help residents navigate Medicaid redeterminations and new eligibility rules. Panelists Sabrina Cawthorne with CAPE, Dr. Pearl Quartey-Kumapley and Patricia Killion with Deaconess, and Mi’Oshia Holloway with Ascension St. Vincent walked participants through new work requirements, more frequent reviews, and looming changes that could push more families off coverage.
From the stage, the word that kept resurfacing was “accountability.” Panelists stressed that under the new rules, able-bodied adults ages 19 to 64 are expected to work or volunteer at least 20 hours a week to keep their Medicaid coverage. The instructions were straightforward: don’t lie on applications, report income accurately, pick up the phone when the state calls, open every letter, and never miss a deadline.
For some on the panel, they argued that everyone who can work should “contribute to the system” so that Medicare, Social Security, and other safety-net programs can survive for those who truly need them. There was quiet frustration with people they believe abuse the system—and a warning that the new rules are aimed at tightening those gaps.
Then a gentleman in the audience took the microphone.
“This is policy violence,” he said. “Health care is a human right. It shouldn’t depend on where you work or whether your boss offers benefits.”
That clash between “accountability” and “policy violence” isn’t just a disagreement in one Evansville room. It is the rationale behind the One Big Beautiful Bill Act, a sweeping federal package enacted in July that has reshaped Medicaid, Medicare, the Children’s Health Insurance Program (CHIP), and ACA subsidies.
Health policy experts describe the law as the steepest rollback of the social safety net since welfare reform in the 1990s. Its provisions include roughly $1 trillion in projected Medicaid cuts and an estimated 16 million people losing coverage. Payment caps will limit how much states can pay hospitals, nursing homes, and doctors to Medicare rates. Pharmacy benefit manager (PBM) reforms, pitched as cost-saving measures, may push more financial pressure onto pharmacies and providers.
Supporters say these changes are needed to reduce fraud and protect the long-term solvency of federal programs. But in rooms like the one at CK Newsome, families, hospital staff, and advocates are already asking a different question: when the safety net is pulled back, who is going to catch the people who fall?
The “Accountability” Side—and its Limits
For people who design or support the new rules, accountability starts with work. Able-bodied adults between 19 and 64 are expected to either work or volunteer at least 20 hours per week to keep their Medicaid coverage. In an article published by GovFacts, of the 7.8 million people projected to lose Medicaid coverage, 4.8 million will lose due to work requirements and the remainder due to increased administrative barriers. Panelists at the forum urged people to take those expectations seriously.
But the reality on the ground in Evansville is more complicated than a simple division between “workers” and “non-workers.” There is a growing group of people who are doing exactly what policymakers say they should—working, sometimes at more than one job—and still find themselves in the coverage gap.
Working but Still at Risk
Some of the people most exposed to the changes are workers at small businesses or non-profit organizations that don’t offer insurance and aren’t large enough to be required to.
Others technically have access to employer plans but can’t afford the premiums or deductibles, especially as federal subsidies for ACA marketplace plans shrink. When rent, food, gas, and childcare are all rising, a few hundred dollars a month for insurance can feel impossible, even for someone who works full time.
For families in this gap, the threat of losing coverage doesn’t just mean skipping a routine checkup. It means putting off mammograms, insulin refills, mental health visits, and blood pressure checks until symptoms become crises. Fear of losing coverage becomes one more reason to avoid care. That delay almost always leads to worse—and more expensive—outcomes later: strokes that might have been prevented, infections that could have been treated earlier, chronic conditions that spiral out of control.
The new rules frame health care as something people earn by meeting work or volunteer requirements and completing paperwork on time. But in practice, the people who fall behind are often those already juggling the most: multiple jobs, unstable schedules, caregiving responsibilities, limited transportation, and little or no paid time off.
Hospitals and Clinics: Caring for Everyone, with Less
ECHO Community Healthcare, Deaconess, Ascension St. Vincent, and other clinics are bracing for what the Big Beautiful Bill could mean in exam rooms and on their balance sheets.
Staff are preparing for an increase in uninsured and underinsured patients, more people arriving in emergency rooms because they’ve lost a primary care provider, and more patients who have gone months or years without preventive care.
Payment caps built into the law will limit how much states can pay hospitals, nursing homes, and doctors for many services, tying rates to Medicare levels that often don’t cover the full cost of care.
“We will take care of people no matter what,” said Dr. Quartey-Kumapley. “That’s who we are. But we don’t yet know how this will hit us—financially, emotionally, or in terms of sheer volume. We’re planning, but a lot of this is unknown.”
Community Response
In the face of these changes, local advocates are trying to build their own kind of safety net. The organizers behind “Medicaid Matters” are working to strengthen a healthcare coalition that brings together clinics, nonprofits, churches, and social service providers.
The goal is simple but ambitious: share information quickly, coordinate community education about policy changes, and make it easier for people to find help filling out forms or appealing terminations. That might mean regular community forums, a shared resource guide, or a network of trusted “navigators” who can walk people through paperwork one-on-one.
At the same time, nonprofits are looking at how volunteer roles might become lifelines. If adults must log 20 hours of work or volunteering each week to keep coverage, organizations are exploring low-barrier options: stocking shelves at food pantries, greeting at community centers, helping with childcare or senior programs, or volunteering at health-focused organizations. The work matters on its own—but now, it could also help people meet insurance requirements.
The One Big Beautiful Bill is here. Its consequences are just beginning to unfold. The policies may be national, but the fallout—and the response—will be decided much closer to home: at kitchen tables, in exam rooms, and even at the CK Newsome.